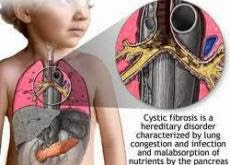
Cystic fibrosis (which is also known as mucoviscidosis) was first described in 1938.
It is an inherited condition in which mucous producing glands throughout the body produce an abnormally thick and sticky form of mucous.
Such glands are present in the lungs, the bowel and the testes.
The thick mucous blocks the outlet from the glands - this causes the glands to dilate and become susceptible to infection and scarring.
The glands cannot perform their normal function and eventually they become ineffective and subject to recurrent infections. Because of this combination of effects, cystic fibrosis causes problems with bowel function and with breathing. Males will have impaired fertility.
What Causes Cystic Fibrosis?
Cystic fibrosis is the most commonly inherited condition of childhood. One in 25 persons is a carrier and it occurs in about 1 in every 3000 births in the UK. Not all children born into a family will be affected since the condition is inherited in an autosomal recessive manner.
What Causes Cystic Fibrosis?
Cystic fibrosis is the most commonly inherited condition of childhood. One in 25 persons is a carrier and it occurs in about 1 in every 3000 births in the UK. Not all children born into a family will be affected since the condition is inherited in an autosomal recessive manner.
This means that both parents need to carry the gene and even then, only one in four children will be affected. Both boys and girls are equally affected. To develop cystic fibrosis, a baby has to inherit two cystic fibrosis genes (one from its mother and one its father).
If a baby inherits one cystic fibrosis gene (from either the mother or father) and one normal gene, the baby will be a 'carrier' and will not develop cystic fibrosis.
Cystic fibrosis is most common in Caucasians. It is uncommon in Asians and in Africans.
What Are The Signs And Symptoms?
There Are Three Different Presentations Of The Cystic Fibrosis Disease:
1. Meconium Ileus:
This form presents at birth with a paralytic obstruction of the bowel, which sometimes perforates. It is caused by blockage of the bowel by the abnormal mucous produced by glands in the bowel wall. The perforation may occur while the baby is still in the mother’s womb, giving rise to peritonitis at the time of birth.
2. Gastro-intestinal:
This form of the disease is usually first noticed between three and eighteen months of life. Because there is a lack of digestive enzymes there is reduced absorption of foodstuffs, particularly fat, fat-soluble vitamins and protein.
Cystic fibrosis is most common in Caucasians. It is uncommon in Asians and in Africans.
What Are The Signs And Symptoms?
There Are Three Different Presentations Of The Cystic Fibrosis Disease:
1. Meconium Ileus:
This form presents at birth with a paralytic obstruction of the bowel, which sometimes perforates. It is caused by blockage of the bowel by the abnormal mucous produced by glands in the bowel wall. The perforation may occur while the baby is still in the mother’s womb, giving rise to peritonitis at the time of birth.
2. Gastro-intestinal:
This form of the disease is usually first noticed between three and eighteen months of life. Because there is a lack of digestive enzymes there is reduced absorption of foodstuffs, particularly fat, fat-soluble vitamins and protein.
There is likely to be diarrhoea (loose, pale, fatty and offensive stools often containing undigested meat and starch granules) and a general failure of the baby to grow properly. Sometimes there may be a small hernia at the tummy button or a prolapse (the sinking down or falling down) of the rectum seen at the anus.
3. Respiratory:
Sooner or later respiratory infections occur because of lack of protective mucous and infection of the glands in the breathing tubes themselves. There is sometimes collapse of a lung, widening of the air-spaces (emphysema) or pneumonia.
3. Respiratory:
Sooner or later respiratory infections occur because of lack of protective mucous and infection of the glands in the breathing tubes themselves. There is sometimes collapse of a lung, widening of the air-spaces (emphysema) or pneumonia.
This group of respiratory symptoms usually start between six and eighteen months of life and may overlap with bowel symptoms.
Will There Be Any Tests Or Investigations?
People with cystic fibrosis produce more concentrated sweat than normal individuals and a ‘sweat test’ is usually used to make the diagnosis. The test is simple, takes only a short time and is usually performed twice.
Will There Be Any Tests Or Investigations?
People with cystic fibrosis produce more concentrated sweat than normal individuals and a ‘sweat test’ is usually used to make the diagnosis. The test is simple, takes only a short time and is usually performed twice.
A small amount of a chemical called pilocarpine is placed on the skin. This causes sweating and the sweat is collected for measurement using a special absorptive dressing. In children with cystic fibrosis the concentration of sodium salt in the sweat is usually above 60mEq/litre.
The diagnosis can be further confirmed by passing a small tube down the throat, through the stomach, and into the duodenum. From there, digestive juices can be sampled. In cystic fibrosis, this juice is thicker than usual and lacking in the normal digestive enzymes.
The diagnosis can be further confirmed by passing a small tube down the throat, through the stomach, and into the duodenum. From there, digestive juices can be sampled. In cystic fibrosis, this juice is thicker than usual and lacking in the normal digestive enzymes.
This is not a hard-and-fast rule however, since normal children may show low levels of digestive enzymes if they have had a recent bowel infection. Other more sophisticated blood tests can also be used to confirm the diagnosis. If the diagnosis is suspected at birth, blood from a heel prick may show an elevated level of an enzyme called trypsin.
Mothers who have had one child with cystic fibrosis will be offered screening tests during subsequent pregnancies to determine whether the child they are carrying is also affected. It is also possible to screen member of the population using cells from the lining of the mouth to determine whether they are carriers of cystic fibrosis.
What Treatment Might Be Necessary For Cystic Fibrosis?
Children with cystic fibrosis should receive at least part of their treatment in a specialist centre where regular monitoring of lung function, digestion and general condition can take place.
If the child is lacking in digestive enzymes, these can be given in the form of granules or capsules with meals. 5-15 grams of these enzymes (known as pancreatin) can be given each day according to the child’s age and this can improve digestion and absorption of protein, fat and other food substances.
Mothers who have had one child with cystic fibrosis will be offered screening tests during subsequent pregnancies to determine whether the child they are carrying is also affected. It is also possible to screen member of the population using cells from the lining of the mouth to determine whether they are carriers of cystic fibrosis.
What Treatment Might Be Necessary For Cystic Fibrosis?
Children with cystic fibrosis should receive at least part of their treatment in a specialist centre where regular monitoring of lung function, digestion and general condition can take place.
If the child is lacking in digestive enzymes, these can be given in the form of granules or capsules with meals. 5-15 grams of these enzymes (known as pancreatin) can be given each day according to the child’s age and this can improve digestion and absorption of protein, fat and other food substances.
To make nutrition more successful, the child’s diet should be made as nourishing as possible with a high protein content. Fatty foods should be avoided but supplements of vitamins and minerals (particularly iron) are useful.
Every effort needs to be made to reduce the likelihood of respiratory symptoms and to treat these early and effectively when they occur.
Every effort needs to be made to reduce the likelihood of respiratory symptoms and to treat these early and effectively when they occur.
These days, the management of children with cystic fibrosis usually takes place at least partly in specialist centres where parents will be taught how to perform regular chest physiotherapy and postural drainage; how to recognise the early signs of infection, and what to do should this occur.
A small and restricted choice of antibiotics is usually recommended for use in cystic fibrosis, in an attempt to reduce the likelihood of resistance to these antibiotics emerging in each individual patient.
Because absorption by mouth is often impaired by bowel problems, antibiotics are sometimes given by nebuliser. An aerosol of the antibiotic is breathed in by the patient over 15 to 30 minutes.
Because absorption by mouth is often impaired by bowel problems, antibiotics are sometimes given by nebuliser. An aerosol of the antibiotic is breathed in by the patient over 15 to 30 minutes.
Alternatively therapy can be delivered directly into the bloodstream through a long-term indwelling catheter. These days these are easy to use and well tolerated.
A new treatment called recombinant Dnase (rhDNase) can be used by nebuliser to break down the thick mucous and reduce the frequency of respiratory infections. Oxygen therapy from a portable cylinder may be needed during severe lung infections.
Because of improved management, patients with cystic fibrosis are now living much longer than ever before and a number of other long-term conditions are emerging. They include diabetes, liver problems, infertility in men and osteoporosis. Each can be treated if and when it occurs.
What Course Will The Illness Follow?
At the present time cystic fibrosis is not curable and treatment is supportive so as to optimise nutrition and growth and prevent recurrent respiratory infections. With modern treatment, children with cystic fibrosis can look forward to many years of enjoyable and high quality life. It is anticipated that 85 percent of children with cystic fibrosis will live to at least 50 years of age.
In some cases, lung problems may become severe. In this situation, lung transplant has revolutionised the outlook. There are other reasons to be optimistic. The gene which is responsible for cystic fibrosis has recently been identified and there is hope that, in the future, new genetic techniques may enable us to develop improved ways of managing the condition or perhaps even finding a cure.
Tell Your Doctor
• if you have had any relatives who have had children with an inherited condition like cystic fibrosis
• if you have any concerns regarding your pregnancy
• if you have any concerns regarding your child’s growth
• if your child has any persistent breathing or bowel symptoms
Ask Your Doctor
• if there is a genetic counselling service in the area
• where the local child development clinic is held
• to ensure your child receives all the normal childhood immunisations including BCG
• where you can get your child weighed and measured regularly
• the telephone number of the health visitor
Because of improved management, patients with cystic fibrosis are now living much longer than ever before and a number of other long-term conditions are emerging. They include diabetes, liver problems, infertility in men and osteoporosis. Each can be treated if and when it occurs.
What Course Will The Illness Follow?
At the present time cystic fibrosis is not curable and treatment is supportive so as to optimise nutrition and growth and prevent recurrent respiratory infections. With modern treatment, children with cystic fibrosis can look forward to many years of enjoyable and high quality life. It is anticipated that 85 percent of children with cystic fibrosis will live to at least 50 years of age.
In some cases, lung problems may become severe. In this situation, lung transplant has revolutionised the outlook. There are other reasons to be optimistic. The gene which is responsible for cystic fibrosis has recently been identified and there is hope that, in the future, new genetic techniques may enable us to develop improved ways of managing the condition or perhaps even finding a cure.
Tell Your Doctor
• if you have had any relatives who have had children with an inherited condition like cystic fibrosis
• if you have any concerns regarding your pregnancy
• if you have any concerns regarding your child’s growth
• if your child has any persistent breathing or bowel symptoms
Ask Your Doctor
• if there is a genetic counselling service in the area
• where the local child development clinic is held
• to ensure your child receives all the normal childhood immunisations including BCG
• where you can get your child weighed and measured regularly
• the telephone number of the health visitor













No comments:
Post a Comment