What Is Heart Failure?
This is the term given to the condition where the heart loses its capacity to pump enough blood through the body to maintain normal body functioning. It usually develops slowly over many years and symptoms vary from slight to severe, depending on how much pumping capacity the heart has lost.
The term 'congestive cardiac failure' (CCF) is often used in connection with this problem but 'congestion' or a build-up of fluid is only one part of heart failure. There are two main types of heart failure;
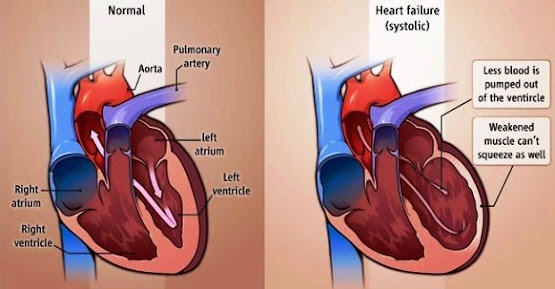
1. Systolic heart failure - the heart does not have sufficient force to push enough blood into the circulation when it contracts.
2. Diastolic heart failure - the heart has trouble relaxing correctly and so becomes stiff and unable to properly fill with blood. It is a condition that increases with increasing age and so is more widely seen in an elderly population.
What Causes Heart Failure?
Apart from age, other factors can contribute to heart failure;
• Smoking
• High blood pressure
• Diabetes
• High cholesterol levels
• Obesity
• Heart valve problems e.g. from previous rheumatic fever.
There may also be some genetic factors which contribute to heart failure but in most instances a specific genetic link is never established.
What Are The Signs And Symptoms Of Heart Failure?
The commonest symptom is shortness of breath. This is often due to fluid collecting in the lungs, and so breathlessness can occur at rest or interrupt normal sleep. Associated with this is fatigue or tiredness since the heart cannot pump sufficient oxygenated blood as 'fuel' to the body, and fluid may also collect in the feet, ankles, legs and abdomen, sometimes causing significant weight gain. Coughing is another sign of heart failure, often with pinky-coloured or frothy sputum. The heart attempts to compensate for failing by adjusting in three ways;
1. It gets bigger
2. The heart muscles become thicker to pump more blood out of it
3. The pulse rate increases to increase the circulation. However, this compensation is not infinite and signs of heart failure appear once these possibilities have been exhausted.
Will I Have Any Tests Or Investigations?
Heart failure is usually suggested at an ordinary clinical examination. A combination of shortness of breath, fluid on the lungs and swollen ankles, and sometimes a raised blood pressure all point to the diagnosis. Confirmatory tests include;
• A chest X-ray. This can show an enlarged heart and the presence of fluid on the lungs.
• An ECG (electrocardiogram) which looks at the electrical activity of the heart, and whether it is under any strain.
• An echocardiogram (ECHO scan) can tell from harmless sound waves being 'bounced' off the heart whether there are any abnormalities in the heart size, shape and movement, and can also assess just how much blood the heart is able to pump out.
• Blood tests are routine, and will include checking for any conditions that could put the heart under strain including anaemia and thyroid problems.
What Treatment Will I Need?
These treatments are both medical and self-help treatments (see below). Medical treatment involves the use of drugs which aim to ease the load on the heart, and which include diuretics ('water tablets'), digitalis and angiotensin converting enzyme (ACE) inhibitors which have been shown to improve heart efficiency in patients with heart failure.
Very rarely, heart failure can become life-threatening - usually when all medical treatments have failed and the heart is unable to compensate any more. In such cases, a heart transplant may be considered but this needs very specialised assessment by cardiac surgeons before a patient is out on the list for such an operation.
What Course Will The Illness Follow?
The majority of people with heart failure are able to lead normal lives, albeit occasionally at a slower pace than in their youth. A steady increase in medication may be necessary with increasing age to maintain the 'status quo' of the heart, along with sensible lifestyle and dietary advice.
1. Systolic heart failure - the heart does not have sufficient force to push enough blood into the circulation when it contracts.
2. Diastolic heart failure - the heart has trouble relaxing correctly and so becomes stiff and unable to properly fill with blood. It is a condition that increases with increasing age and so is more widely seen in an elderly population.
What Causes Heart Failure?
Apart from age, other factors can contribute to heart failure;
• Smoking
• High blood pressure
• Diabetes
• High cholesterol levels
• Obesity
• Heart valve problems e.g. from previous rheumatic fever.
There may also be some genetic factors which contribute to heart failure but in most instances a specific genetic link is never established.
What Are The Signs And Symptoms Of Heart Failure?
The commonest symptom is shortness of breath. This is often due to fluid collecting in the lungs, and so breathlessness can occur at rest or interrupt normal sleep. Associated with this is fatigue or tiredness since the heart cannot pump sufficient oxygenated blood as 'fuel' to the body, and fluid may also collect in the feet, ankles, legs and abdomen, sometimes causing significant weight gain. Coughing is another sign of heart failure, often with pinky-coloured or frothy sputum. The heart attempts to compensate for failing by adjusting in three ways;
1. It gets bigger
2. The heart muscles become thicker to pump more blood out of it
3. The pulse rate increases to increase the circulation. However, this compensation is not infinite and signs of heart failure appear once these possibilities have been exhausted.
Will I Have Any Tests Or Investigations?
Heart failure is usually suggested at an ordinary clinical examination. A combination of shortness of breath, fluid on the lungs and swollen ankles, and sometimes a raised blood pressure all point to the diagnosis. Confirmatory tests include;
• A chest X-ray. This can show an enlarged heart and the presence of fluid on the lungs.
• An ECG (electrocardiogram) which looks at the electrical activity of the heart, and whether it is under any strain.
• An echocardiogram (ECHO scan) can tell from harmless sound waves being 'bounced' off the heart whether there are any abnormalities in the heart size, shape and movement, and can also assess just how much blood the heart is able to pump out.
• Blood tests are routine, and will include checking for any conditions that could put the heart under strain including anaemia and thyroid problems.
What Treatment Will I Need?
These treatments are both medical and self-help treatments (see below). Medical treatment involves the use of drugs which aim to ease the load on the heart, and which include diuretics ('water tablets'), digitalis and angiotensin converting enzyme (ACE) inhibitors which have been shown to improve heart efficiency in patients with heart failure.
Very rarely, heart failure can become life-threatening - usually when all medical treatments have failed and the heart is unable to compensate any more. In such cases, a heart transplant may be considered but this needs very specialised assessment by cardiac surgeons before a patient is out on the list for such an operation.
The majority of people with heart failure are able to lead normal lives, albeit occasionally at a slower pace than in their youth. A steady increase in medication may be necessary with increasing age to maintain the 'status quo' of the heart, along with sensible lifestyle and dietary advice.
Patients with heart failure should inform their doctor of any significant change in their condition such as a worsening in their breathing or swelling of their feet.
Can I Do Anything To Help Myself?
A great deal, the main ones being;
• Stopping smoking - essential.
• Losing weight if necessary
• Avoiding alcohol
• Reducing the amount of salt in the diet
• Regular, modest amounts of exercise
• Taking medication as prescribed
• Strictly controlling any high blood pressure or diabetes
• Eating a low-fat diet if your blood cholesterol level is high.
All these factors are essential in the fight against heart disease of any nature and will go a very great way in helping your heart be placed under less strain as a result.
Tell Your Doctor
1. Have you noticed your ankles swelling recently?
2. Do you get short of breath very easily when exercising or when lying down?
3. Are you more tired than usual?
4. Do you have any pain in your chest?
5. Have you noticed any palpitations or odd heart 'bumping' recently?
Ask Your Doctor
1. How mild or otherwise is my heart failure?
2. Will it ever get better to any degree by itself?
3. Am I allowed to fly?
4. Am I at more risk of a heart attack?
5. What are the side effects of my medication?
Useful Contacts
British Heart Foundation
Address: Lyndon Place, 2096 Coventry Road, Sheldon, Birmingham, B26 3YU, UK
Phone Helpline: 0300 330 3311
Contact Form: www.bhf.org.uk/about-us/contact-us
Website: www.bhf.org.uk
The Cardiomyopathy Association
Address: Unit 10, Chiltern Court, Asheridge Road, Chesham, Bucks, HP5 2PX, UK
Telephone: +44 1494 791224
Website: www.cardiomyopathy.org
Can I Do Anything To Help Myself?
A great deal, the main ones being;
• Stopping smoking - essential.
• Losing weight if necessary
• Avoiding alcohol
• Reducing the amount of salt in the diet
• Regular, modest amounts of exercise
• Taking medication as prescribed
• Strictly controlling any high blood pressure or diabetes
• Eating a low-fat diet if your blood cholesterol level is high.
All these factors are essential in the fight against heart disease of any nature and will go a very great way in helping your heart be placed under less strain as a result.
Tell Your Doctor
1. Have you noticed your ankles swelling recently?
2. Do you get short of breath very easily when exercising or when lying down?
3. Are you more tired than usual?
4. Do you have any pain in your chest?
5. Have you noticed any palpitations or odd heart 'bumping' recently?
Ask Your Doctor
1. How mild or otherwise is my heart failure?
2. Will it ever get better to any degree by itself?
3. Am I allowed to fly?
4. Am I at more risk of a heart attack?
5. What are the side effects of my medication?
Useful Contacts
British Heart Foundation
Address: Lyndon Place, 2096 Coventry Road, Sheldon, Birmingham, B26 3YU, UK
Phone Helpline: 0300 330 3311
Contact Form: www.bhf.org.uk/about-us/contact-us
Website: www.bhf.org.uk
The Cardiomyopathy Association
Address: Unit 10, Chiltern Court, Asheridge Road, Chesham, Bucks, HP5 2PX, UK
Telephone: +44 1494 791224
Website: www.cardiomyopathy.org



















No comments:
Post a Comment